Bunions are a common foot condition characterized by a bony prominence that develops at the base of the big toe, often causing discomfort and changes in foot alignment. While they may appear similar, bunions can vary in type, severity, and underlying cause. Understanding the different types of bunions helps individuals recognize symptoms early and explore appropriate treatment options to maintain foot health and mobility.
1. Hallux Valgus
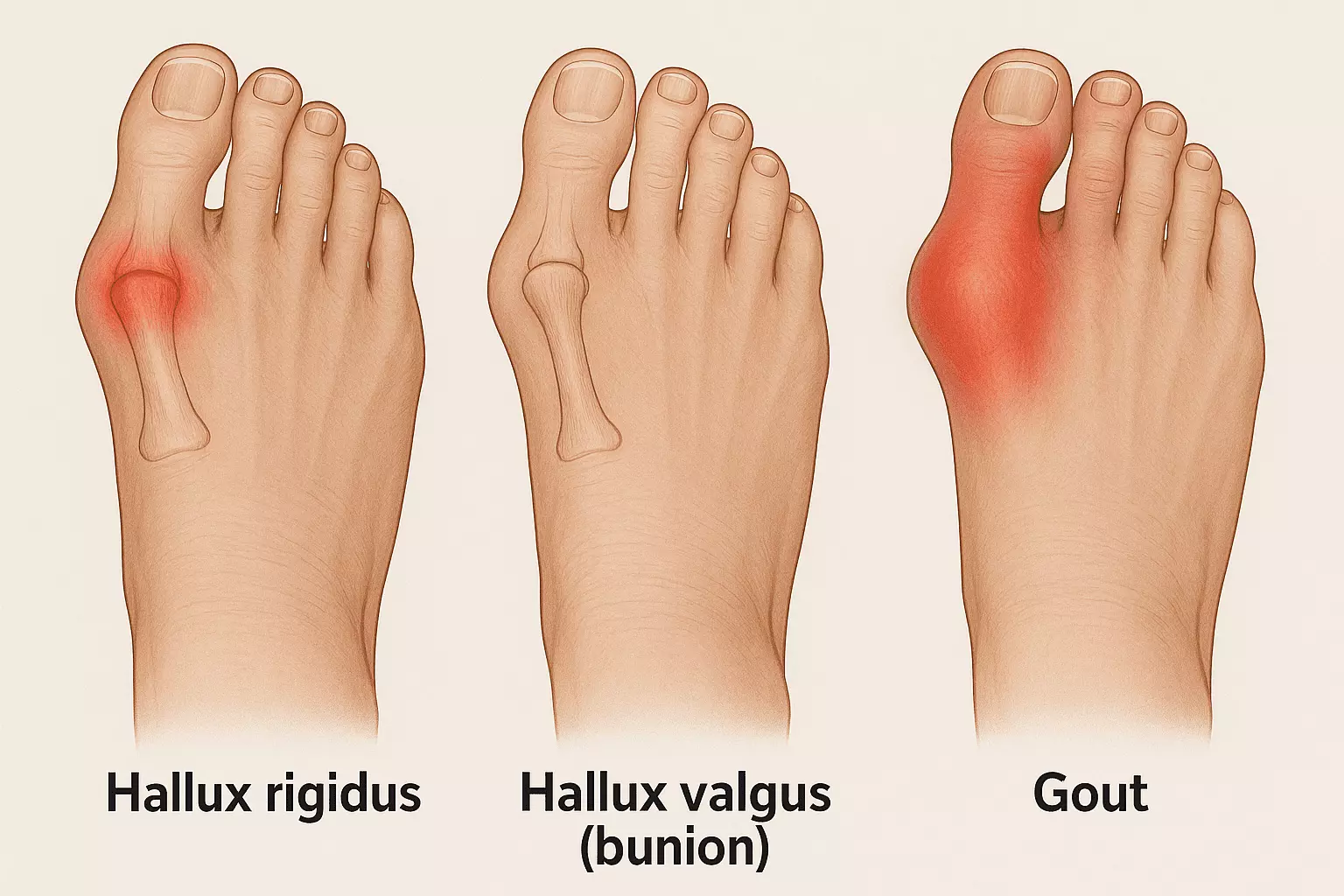
Hallux valgus is the most common type of bunion, also known as the Classic Big Toe Bunions. It affects the joint at the base of your big toe. This causes the toe to lean inward toward your smaller toes. As it drifts, the bone shifts outward, creating a bump. You might notice redness, swelling, or pain after wearing tight shoes. While footwear matters, genetics play a major role in its development.
You will often manage early symptoms with conservative care. Try switching to shoes with a wide toe box to relieve pressure. Custom orthotics also help stabilize your foot mechanics. If the deformity becomes severe, correction becomes necessary. A qualified clinic uses advanced 3D, minimally invasive techniques to achieve better results. This approach realigns the bone with less soft-tissue trauma and is designed to speed recovery.
2. Tailor’s Bunion (Bunionette)
A bunion doesn’t just form on the big toe; it can also develop on the outside edge of the foot. This variation, called a “bunionette,” forms at the base of the little toe and is much smaller than a traditional bunion. Its nickname, “Tailor’s bunion,” comes from tailors who sat cross-legged for hours, pressing the outside of their feet against the ground. Today, narrow shoes are a major cause, as they squeeze the toes together and create friction on the fifth metatarsal bone.
Treating a Tailor’s bunion starts with modifying footwear to reduce friction in the affected area. Adding padding can help relieve discomfort, but addressing the structural issue is key to long-term foot health. Since this part of the foot has little natural padding, even small bunionettes can cause significant pain when they rub against shoes.
3. Congenital and Juvenile Bunions
Many believe bunions only affect older adults. However, juvenile bunions appear in children and teenagers, usually due to genetics. A young person might inherit flat feet or loose ligaments, leading to foot instability. Because their bones are still developing, early evaluation is necessary. This helps manage the condition before it worsens. Juvenile cases are often flexible, but they sometimes cause pain during sports.
Surgery is rarely the first choice for adolescents. There is a high risk that the bunion could return as they grow. Instead, treatment focuses on monitoring and managing symptoms. Custom orthotics are a helpful tool for children. They correct foot position and slow the deformity’s progression. Taking these practical steps helps kids stay active and comfortable.
4. Arthritic and Inflammatory Bunions
Systemic health issues can sometimes cause painful foot deformities, such as bunions, which are linked to rheumatoid arthritis. This autoimmune disease attacks joint linings, often leading to severe bunion deformities that are harder to manage. These inflammatory bunions are symptoms of a larger problem and may cause stiffness and aching unrelated to shoe pressure. Additionally, conditions like gout can mimic bunion pain or worsen an existing structural issue due to inflammation.
Treating inflammatory bunions requires addressing both the foot structure and the underlying arthritis. Collaboration with a rheumatologist and a foot and ankle surgeon is key to managing the inflammation effectively. Surgery is sometimes necessary to reconstruct the joint and restore foot function. This comprehensive approach helps alleviate pain and improve mobility for patients.
Schedule Your Foot Evaluation Today
Foot pain should not prevent you from carrying out your daily outdoor activities. Whether you are dealing with a classic Hallux valgus or a smaller bunionette, professional intervention from a skilled podiatrist is helpful for long-term mobility. Consult a clinic and a surgeon who specializes in both conservative care and advanced, minimally invasive surgery to correct these issues.
Early treatment often prevents the need for surgery and keeps you active for years to come. Book a consultation with a podiatrist near you to gain clarity about your condition.
