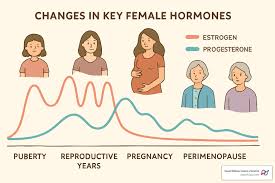
Menopause marks a significant biological transition in a woman’s life, signaling the end of her reproductive years. This process is officially confirmed when a woman has gone 12 consecutive months without a menstrual period, and it typically occurs between the ages of 45 and 55. The driving force behind this transition is a natural decline in ovarian hormone production. As women age, the ovaries produce less estrogen and progesterone, the primary hormones that regulate the menstrual cycle. Estrogen supports bone health and cholesterol, while progesterone prepares the uterus for pregnancy. When these hormone levels fluctuate and eventually drop, the body undergoes various physical and emotional adjustments. Women can consult a hormone specialist during this time for guidance and support.
Common Symptoms
Lower estrogen and progesterone impact many body systems, causing symptoms that differ in intensity for each person. While some women experience mild discomfort, others may find these changes disruptive to their daily routines. One of the most recognizable signs is hot flashes. These are sudden feelings of intense heat that spread over the upper body and face, and they are often accompanied by sweating and a rapid heartbeat. Night sweats are hot flashes that occur during sleep and can lead to significant sleep disturbances and fatigue.
Other common symptoms include:
- Vaginal Dryness: Lower estrogen levels can cause vaginal tissues to become thinner and drier, leading to discomfort or pain during intercourse.
- Mood Changes: Fluctuating hormones may contribute to irritability, anxiety, or feelings of sadness.
- Weight Gain: Many women notice a slowing metabolism, which often results in weight gain, particularly around the abdomen.
- Sleep Problems: Difficulty falling asleep or staying asleep is frequently reported, often due to night sweats or general discomfort.
- Thinning Hair and Dry Skin: Estrogen loss can reduce collagen production, affecting skin elasticity and hair volume.
Symptom Duration
The duration of menopause and its associated symptoms is highly individual and can span several years. The entire transition is often divided into three stages: perimenopause, menopause, and postmenopause. Perimenopause is the transitional phase leading up to menopause, and it can begin several years before the final menstrual period. During this time, hormone levels fluctuate unpredictably, and symptoms often begin to appear.
The average length of perimenopause is about four years, but for some women, it may last only a few months or extend up to a decade. Once a woman has not had a period for 12 months, she enters postmenopause. While some symptoms, like hot flashes, may improve over time, the lower hormone levels are permanent. This means that certain health risks associated with low estrogen, such as osteoporosis or heart disease, may increase as women age.
Treatment Options
Managing menopausal symptoms focuses on relieving discomfort and maintaining overall health. There is no single approach that works for everyone, so treatment plans are often personalized based on symptom severity and medical history. Lifestyle adjustments may make a significant difference for many women. Regular exercise supports bone health, helps manage weight, and can improve mood and sleep quality. A balanced diet rich in calcium and vitamin D is recommended for protecting bones. Avoiding triggers like caffeine, alcohol, and spicy foods may help reduce the frequency of hot flashes.
Medical treatments are also available for those with more severe symptoms. Hormone therapy involves taking estrogen (and often progestin) to replace the hormones the body is no longer producing in sufficient quantities. This can be effective for hot flashes and bone loss, but it is not suitable for everyone. Non-hormonal medications like some antidepressants or those for hot flashes provide options for women avoiding taking hormones. Vaginal estrogen creams or lubricants may specifically address localized dryness and discomfort.
Ask a Hormone Specialist Today
Navigating the changes of menopause may be challenging, and a hormone specialist or a gynecologist can provide expert guidance tailored to your specific needs. They can evaluate your hormone levels, discuss your symptoms in detail, and help you weigh the benefits and risks of different treatment options. Scheduling a consultation helps you receive accurate information and a care plan designed to support your long-term well-being.
